RESEARCH INTERESTS
Circulating immune cells must exit blood vessels near specific target sites of injury, inflammation or tissue repair. The vessel wall at these sites displays specific combinations of traffic signals which operate in sequence to recruit only specific circulating subsets with proper receptors to these signals. As these processes take place under shear stress, we use special flow chambers which simulate blood flow and intravital microscopy in genetically manipulated mice, together with state of the art 3D imaging techniques, to dissect how endothelial and perivascular trafficking molecules promote context- and tissue- selective exit of immune cells through distinct blood vessels.
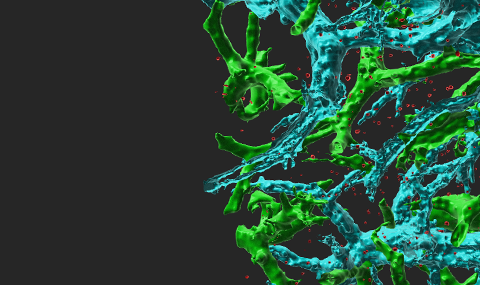
We are also interested in how the leukocyte nucleus manages to squeeze through small confinements, such as endothelial gaps, pores, and additional mechanical barriers, that immune cells encounter after they cross blood vessels on their way to their final targets in the tissues. Recently, we began comparing nuclear squeezing of leukocytes vs. tumor cells and found substantial differences in the molecular signatures used by immune cells and by solid tumor cells to transmigrate through endothelial barriers. We also study how chemotactic and antigenic signals promote the stoppage of lymphocytes on dendritic cells and macrophages during distinct infectious processes and vaccinations. We follow how specific subsets of lymphocytes use adhesion signals to undergo differentiation into efficient effector cells and how these cells acquire memory, one of the most fundamental questions in immunological research. This information is key for the development of novel therapeutic tools for inflammatory disorders, such as autoimmune diseases, atherosclerosis and organ rejection.
A new avenue of research in our lab is dedicated to lung metastasis, and in particular to the intimate communication between circulating cancer cells entering the pulmonary capillaries and blood constituents like platelets, neutrophils, T cells, NK cells and other leukocytes. Circulating cancer cells are either eliminated by this communication or harness specific cellular components that facilitate their crossing of lung vessels and subsequent metastasis.